Implants
When Dental Implants Are Indicated
Dental implants are considered when a tooth is missing or cannot be predictably restored, and when preserving adjacent tooth structure is a priority. They provide a fixed, long-term solution that restores function, supports the surrounding bone, and integrates naturally within the dentition.
Candidacy is determined by bone quality and quantity, periodontal health, occlusion, and systemic factors. When these conditions are favorable, implants can offer a stable, biologically sound foundation for single-tooth replacement, fixed prostheses, or implant-supported overdentures.
Why Dental Implants are Preferred
Dental implants replace the tooth at its root. This allows forces to be transferred to the surrounding bone, helping preserve bone volume and maintain facial structure over time. In contrast, alternatives like bridges or removable prostheses do not provide the same stimulus to the bone.
They are also independent of adjacent teeth. Unlike a traditional bridge, implants do not require preparation of neighboring teeth, preserving natural tooth structure and simplifying long-term maintenance.
Process and Healing
Implant therapy is completed in phases to allow for biologic integration. After placement, the implant body is given time to heal within the bone (osseointegration) over several months. During this period, the surrounding bone adapts and stabilizes around the implant surface.
Once integration is confirmed, the final restoration is designed and placed to restore form and function. Healing timelines vary based on anatomy, bone quality, and overall health.
Implant Health
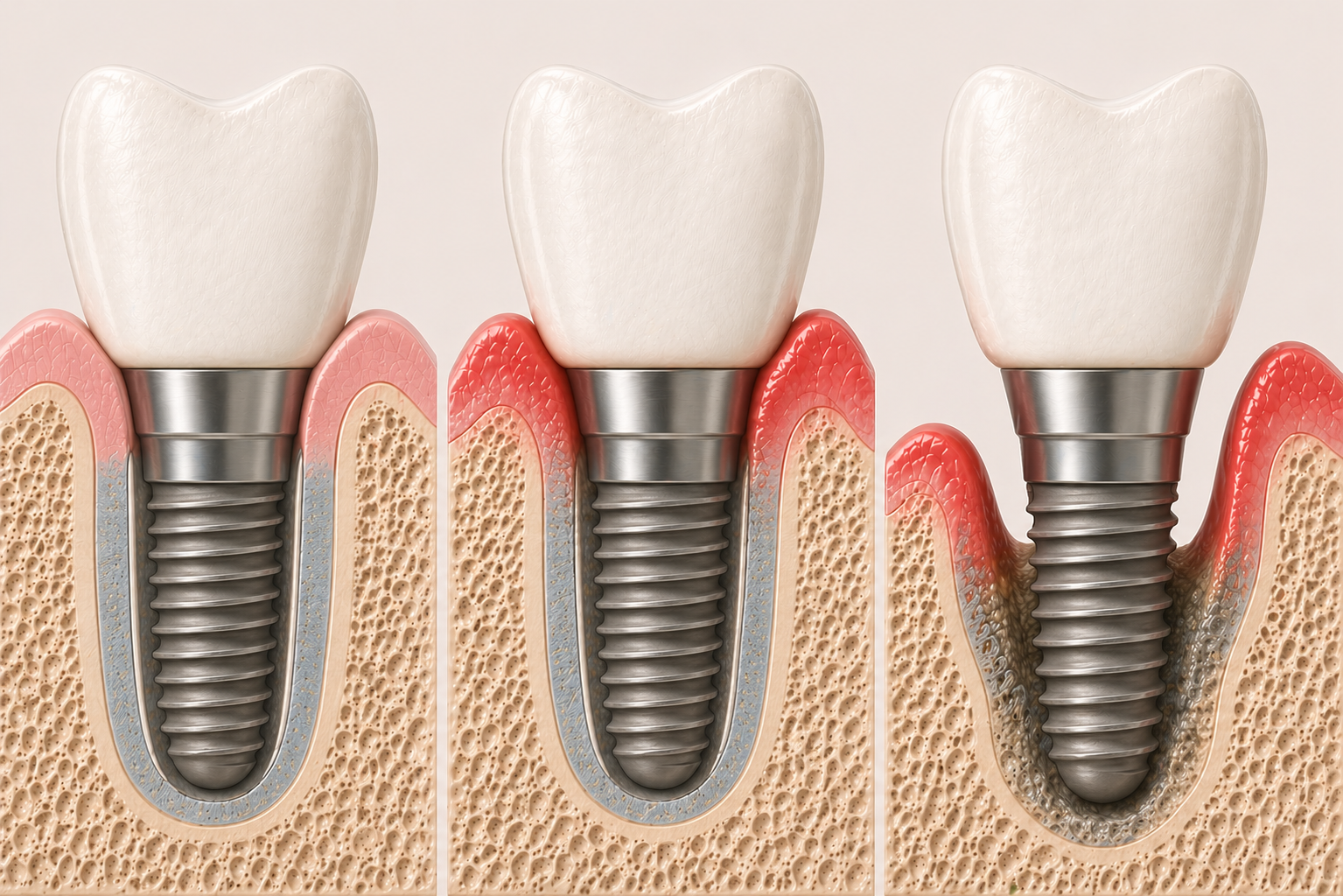
Dental implants do not decay, but they are not immune to disease. The surrounding tissues remain biologically active and susceptible to inflammation. Unlike natural teeth, implants lack a periodontal ligament and have a different connective tissue attachment. This alters both vascular supply and immune response, making early disease progression more subtle and, at times, more rapid.
Peri-implant health is defined by the absence of inflammation and the preservation of stable bone levels. When inflammation is present without associated bone loss, the condition is termed peri-implant mucositis. In contrast, peri-implantitis is characterized by inflammation accompanied by progressive loss of supporting bone.
Disease is driven by complex microbial biofilms, similar to periodontal disease, but implants are often more vulnerable due to their structural differences. Risk factors include a history of periodontal disease, inadequate oral hygiene, excess cement, and biomechanical overload.
Because implants lack the same sensory feedback as natural teeth, complications may not be immediately apparent to the patient. For this reason, evaluation must be deliberate and ongoing, incorporating clinical examination and radiographic comparison over time.
Important Considerations
Timing is critical. Implants should not be placed until skeletal growth has stabilized, as continued development can alter position over time.
Orthodontic treatment often precedes implant placement to establish proper spacing and alignment.
Candidacy is guided by bone quality and volume; site development (e.g., bone grafting) may be recommended when needed.
Periodontal health must be stable prior to placement, with ongoing maintenance to reduce risk of complications.
Occlusion and parafunctional habits (e.g., clenching, grinding) are evaluated as part of treatment planning.
Systemic and lifestyle factors (e.g. smoking, diabetes, and certain medications) can influence healing and integration.
Long-term success depends on regular professional maintenance and consistent home care.
